In recent years, high blood pressure — or hypertension — has quietly climbed the ranks as one of the most critical public health concerns worldwide. Often dubbed “the silent killer,” it contributes to heart disease, stroke, kidney failure, and even cognitive decline. And now, with updated medical guidelines lowering the threshold for what’s considered “high,” millions more people may find themselves newly diagnosed — or newly motivated to take action.
The American Heart Association and American College of Cardiology revised their guidelines in 2017, redefining high blood pressure as 130/80 mm Hg or higher, down from the previous benchmark of 140/90. This shift means nearly half of U.S. adults — and similar proportions globally — now fall into the hypertensive category. The message is clear: blood pressure matters more than ever, and managing it is no longer optional — it’s essential.
But with so many factors influencing blood pressure, where should you start? What truly moves the needle? Here’s what science says is most important — and how to get there.
Lifestyle Is the First Line of Defence
Before reaching for a prescription, experts agree: lifestyle changes are the most powerful, sustainable way to lower blood pressure — and often, they’re enough on their own.
- Move More, Sit Less
Regular physical activity can lower systolic blood pressure (the top number) by 5 to 8 mm Hg. Aim for at least 150 minutes per week of moderate aerobic exercise — brisk walking, cycling, or swimming. Even short bursts of movement throughout the day help counteract the effects of prolonged sitting.
- Eat for Your Heart
The DASH (Dietary Approaches to Stop Hypertension) diet remains the gold standard. It emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting sodium, saturated fats, and added sugars. Reducing sodium intake to less than 2,300 mg per day — ideally 1,500 mg — can lower blood pressure significantly, especially in salt-sensitive individuals.
- Shed Excess Weight
Even losing 5–10 pounds can make a measurable difference. Fat, particularly around the abdomen, increases resistance in blood vessels and strains the heart. Weight loss eases that burden — and often improves sleep, insulin sensitivity, and inflammation, too.
- Limit Alcohol and Quit Smoking
More than one drink per day for women or two for men can raise blood pressure. And while smoking doesn’t directly cause chronic hypertension, it damages blood vessels, accelerates arterial stiffness, and multiplies cardiovascular risk.
- Stress Isn’t Just in Your Head — It’s in Your Arteries
Chronic stress triggers the release of hormones like cortisol and adrenaline, which constrict blood vessels and elevate heart rate — both of which spike blood pressure. While you can’t eliminate stress entirely, you can change how you respond to it.
- Practice mindfulness, meditation, or deep breathing for 10–15 minutes daily.
- Prioritise sleep — aim for 7–9 hours per night. Poor sleep disrupts hormonal balance and increases sympathetic nervous system activity, both of which raise pressure.
- Consider yoga or tai chi — movement paired with breathwork has proven benefits for lowering BP.
Medication When Needed — No Shame, Just Strategy
For some, lifestyle changes alone aren’t enough — especially if blood pressure is significantly elevated or other risk factors (like diabetes or kidney disease) are present. That’s where medication comes in.
Common first-line drugs include:
- ACE inhibitors and ARBs — relax blood vessels
- Calcium channel blockers — prevent artery constriction
- Diuretics — reduce fluid volume
The goal isn’t just to hit a number — it’s to protect your organs and extend your health span. Work with your doctor to find the right medication and dosage. Don’t stop or adjust meds without medical guidance — consistency is key.
Monitor at Home — Knowledge Is Power
White-coat hypertension (elevated readings at the doctor’s office) and masked hypertension (normal in-office, high at home) are real phenomena. Home monitoring gives you — and your doctor — a clearer picture.
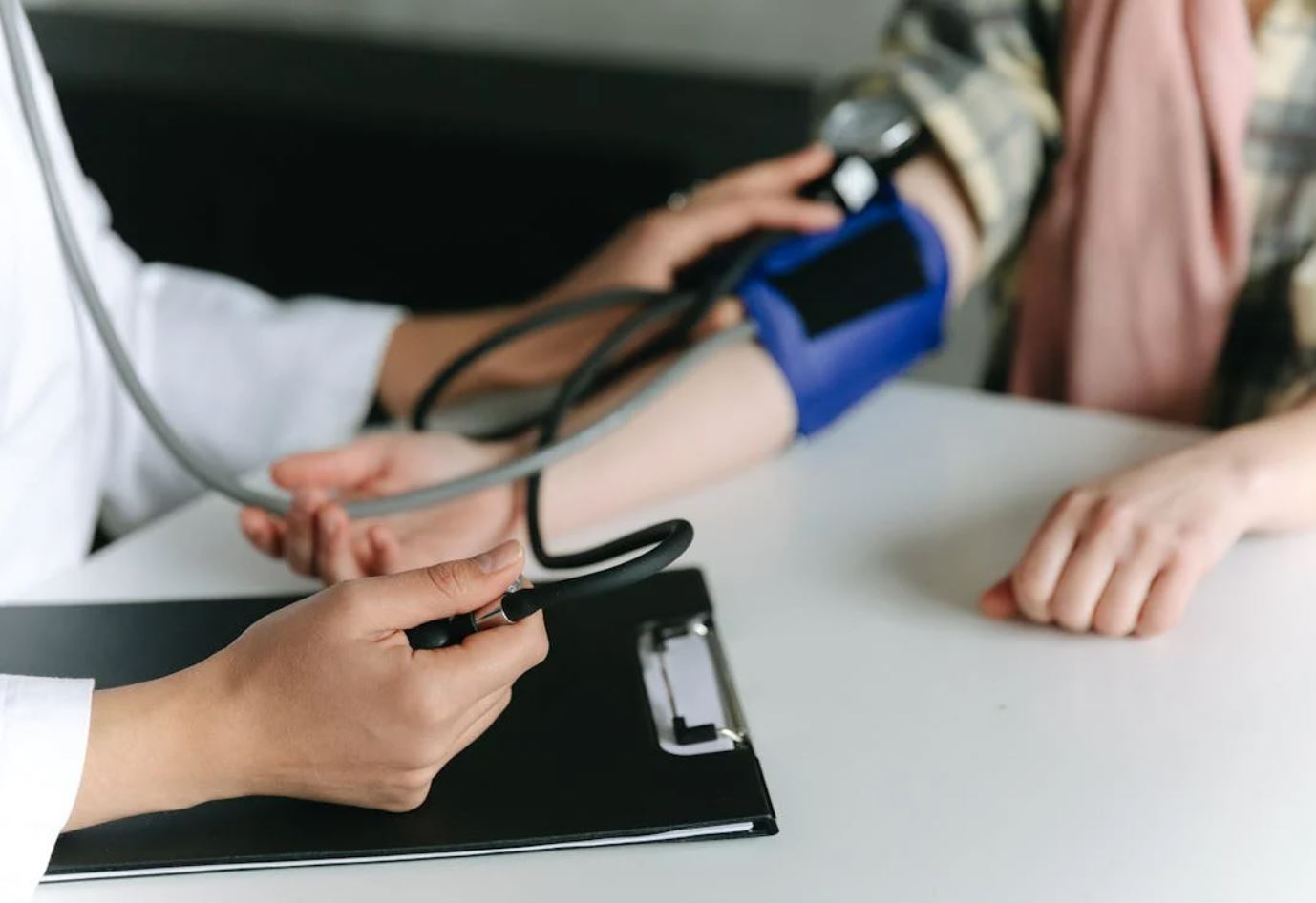
Invest in a validated, upper-arm cuff monitor. Take readings at the same time each day, seated and relaxed, after 5 minutes of quiet. Keep a log. Trends matter more than single readings.
Community, Consistency, and Compassion
Lowering blood pressure isn’t a sprint — it’s a lifelong practice. Setbacks happen. Progress is rarely linear. The most successful patients treat this as a holistic journey: nourishing their bodies, calming their minds, and leaning on support systems.
Join a walking group. Cook healthy meals with family. Celebrate small wins — like choosing fruit over chips or taking the stairs. Every positive choice compounds.
The Bottom Line
Blood pressure isn’t just a number on a chart — it’s a window into your cardiovascular future. With tighter guidelines, we’re being asked to pay attention sooner and act more decisively. But the tools to succeed are within reach: movement, mindful eating, rest, stress management, and when needed, medication.
Start today. Pick one change — just one — and build from there. Because when it comes to your heart, every point counts.
Talk to your healthcare provider before making significant lifestyle changes or adjusting medications. Individual needs vary — your plan should, too.
