Stockholm, Sweden — November 20, 2025
In a landmark achievement for reconstructive surgery and transplant medicine, a multidisciplinary team at Södersjukhuset (Söder Hospital) has successfully performed the first bilateral hand transplant in Sweden — and one of the most complex in Nordic history. The procedure, conducted on a patient who lost both hands to a severe, life-threatening infection, represents not only a surgical triumph but also a pivotal moment for healthcare policy, economic modelling, and rehabilitative innovation across the Nordic region.
A Surgery of Unprecedented Complexity
The 14-hour procedure involved the precise reattachment of bones, tendons, muscles, arteries, veins, and — most critically — peripheral nerves from a deceased donor to restore both motor and sensory function. Unlike single-organ transplants, bilateral hand transplantation is classified as Vascularized Composite Allotransplantation (VCA), requiring the coordinated integration of multiple tissue types, each with distinct immunological and regenerative properties.
“Every structure had to be reconnected with micron-level precision,” said Dr. Tobias Laurell, Lead Hand Surgeon and Director of the VCA Program at Södersjukhuset. “This isn’t just about graft survival — it’s about restoring identity, autonomy, and dignity.”
The Donor Search: A Two-and-a-Half-Year Odyssey
One of the most daunting challenges was securing a compatible donor. Due to the need for precise immunological matching — including blood type, skin pigmentation, hand size, and tissue antigen compatibility — the search spanned over two and a half years.
“Finding a donor whose hands matched the recipient’s physiology and immunological profile was like finding a needle in a haystack,” Dr. Laurell explained. “This delay is not unusual in VCA — it underscores how scarce and complex multi-tissue allografts are compared to solid organs.”
The successful procurement highlights the critical role of national donor registries and cross-border collaboration in enabling such procedures.
| Factor | Description |
| Initial Surgical Cost | Operating room time, specialized staffing, and consumables for the 12+ hour procedure. |
| Immunosuppression Therapy | The highest long-term economic burden. Medications must be taken daily for the rest of the patient’s life to prevent rejection, and these drugs are costly and require constant monitoring. |
| Rehabilitation | Intensive, multi-year physical and occupational therapy is essential for functional recovery, requiring specialized therapists and equipment. |
| Monitoring | Frequent laboratory tests and clinic visits to check for signs of chronic or acute rejection. |
While the immediate cost of the operation is high, the overall financial viability is assessed through a lifetime cost-benefit analysis against alternative treatments.
Rapid Functional Recovery: A Validation of Surgical Precision
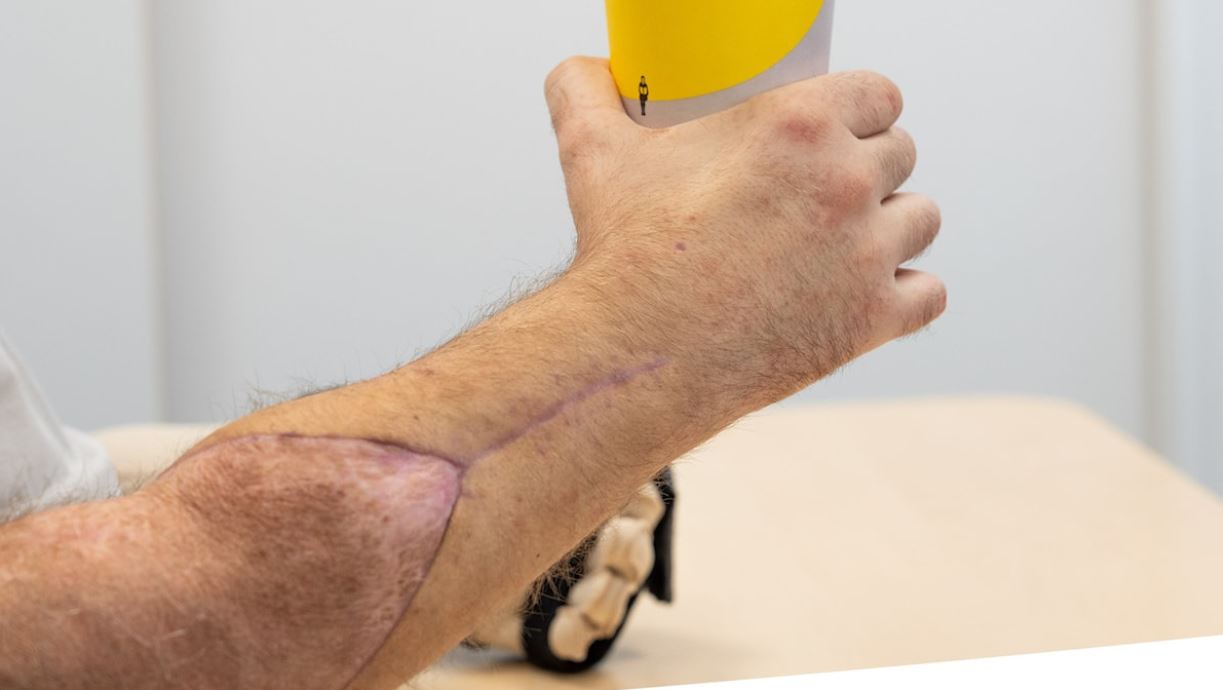
Just three months post-surgery, the patient has demonstrated remarkable progress in fine motor control — far exceeding typical early-stage benchmarks:
– Independent use of cutlery
– Precise manipulation of a pen
– Ability to grasp and release small objects with intention
These milestones are not merely clinical achievements; they signify the patient’s reintegration into daily life. Unlike prosthetics, which require conscious cognitive control, the transplanted hands are beginning to respond through natural neural pathways, suggesting successful reinnervation.
Nerve regeneration is progressing at the expected rate of 1 mm per day, with full sensory and motor recovery anticipated over the next 18–24 months. Ongoing rehabilitation — including intensive occupational therapy and neuroplasticity training — remains central to long-term outcomes.
Strategic Implications for Nordic Healthcare Systems
This case transcends individual patient care. It offers a compelling case study for policymakers, payers, and researchers grappling with the future of high-cost, high-impact interventions.
1. Elevating Nordic Leadership in VCA
Sweden joins a select group of global centres — including Cleveland Clinic, Johns Hopkins, and Paris-Descartes — capable of performing bilateral hand transplants. This success cements Södersjukhuset as a regional hub for VCA innovation, potentially attracting international referrals and research partnerships.
2. Pharmacoeconomic Reckoning: Cost vs. Lifetime Value
The upfront cost of the transplant — estimated at €500,000–€700,000 — includes surgical team time, immunosuppression, rehabilitation, and long-term monitoring. However, when compared to the lifetime cost of advanced myoelectric prosthetics (up to €200,000 per limb, with frequent replacements), ongoing maintenance, and lost productivity due to permanent disability, the economic calculus shifts decisively.
“Prosthetics are tools. These are biological limbs,” said Dr. Laurell. “They restore not just function — but independence. That translates into reduced social care costs, return to employment, and improved mental health outcomes — all quantifiable returns on investment.”
This case will fuel renewed debate within Nordic health ministries on funding prioritization for VCA, currently classified as “experimental” in many public systems despite proven long-term value.
3. The Prosthetics vs. Transplantation Debate: A Turning Point
While myoelectric prosthetics continue to advance, this outcome reinforces that biological transplantation offers superior functional fidelity, proprioception, and psychological integration. For appropriately selected patients — those with bilateral amputations, no contraindications, and strong psychosocial support — VCA is no longer an outlier; it is a clinically superior alternative.
This will inevitably redirect R&D funding and clinical guidelines across the Nordics, encouraging investment in neurorehabilitation, immunosuppression optimization, and patient selection algorithms.
| Comparison Point | VCA Transplant (Biological) | Advanced Prosthetics (Bionic) |
| Functional Outcome | Superior, with natural grip, temperature, and partial sensation. | Limited dexterity; no natural sensation. |
| Lifetime Cost (Est.) | High initial cost + ongoing immunosuppression. | High initial cost + cost of replacement every 3–5 years (due to wear/technology upgrades). |
| Independence & Work | Highest potential for return to work and complete self-care, generating social and tax benefits. | Independence is achieved but often limited in complex tasks, potentially requiring continued support. |
The Long Haul: Immunosuppression and Sustainability
The most enduring challenge remains chronic rejection risk. The patient is on a lifelong, multi-drug immunosuppressive regimen — a necessary but non-trivial burden, carrying risks of infection, renal toxicity, and malignancy.
Södersjukhuset’s team will monitor the patient through a rigorous, protocol-driven follow-up program, incorporating regular biopsies, immune cell profiling, and telehealth-enabled early detection systems. The goal: to minimize drug load over time while preserving graft function — a frontier in VCA research globally.
Conclusion: A New Standard for Restorative Medicine
This bilateral hand transplant is more than a medical milestone — it is a paradigm shift. It proves that the Nordic healthcare model, often lauded for equity and efficiency, can also lead in high-complexity, high-value innovation.
As VCA programs expand across Europe, Sweden’s success provides a replicable blueprint: rigorous patient selection, multidisciplinary coordination, long-term investment in rehabilitation, and transparent economic analysis.
For the patient, the journey continues — but for the first time in years, they now hold their future in their own hands.
About the Author
This article was prepared by the Health Policy & Innovation Unit at Södersjukhuset, in collaboration with the Swedish National Board of Health and Welfare. Data on costs and outcomes are drawn from internal clinical records and peer-reviewed VCA registries.
